From Fear to Happy Recovery: The Impact of Laparoscopy in Colon Cancer Surgery (Discharged on Day 5 After Major Surgery)
An elderly patient presented with abdominal pain and anemia, raising concern for an underlying gastrointestinal pathology. At an earlier stage, the patient had refused colonoscopy and biopsy due to fear of pain and the possibility of major surgery.
With progression of symptoms, the need for evaluation became essential. After detailed counselling and reassurance, the patient agreed to undergo colonoscopy and biopsy, which confirmed carcinoma of the colon. With further reassurance and discussion, the patient subsequently consented to definitive surgical management.
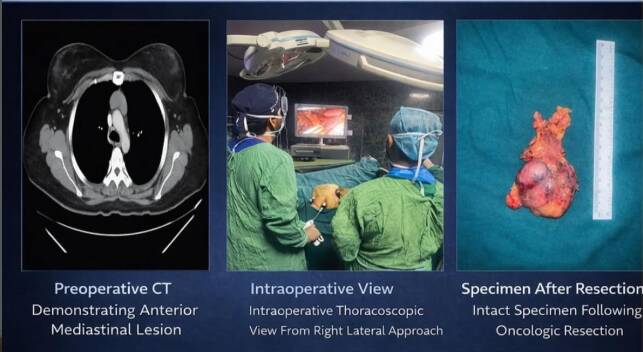
The patient underwent a laparoscopic radical hemicolectomy. This minimally invasive approach ensured adequate oncological clearance while significantly reducing surgical trauma.
The recovery was remarkable. Despite undergoing major cancer surgery, the patient experienced minimal pain, early mobilisation, and was discharged on postoperative day 5 in stable condition.
For this patient, laparoscopy truly transformed the experience of cancer surgery—turning fear into confidence and leading to a smooth, happy recovery.
💡 Key Message
Fear often delays diagnosis and treatment in colon cancer. With advances in laparoscopic surgery, even major procedures can now be performed with less pain, faster recovery, and excellent outcomes.
From fear to happy recovery — this is the real impact of laparoscopy in modern cancer surgery.
📞 Contact
Dr. Pavan Kumar C. G.
Consultant Surgical Oncologist
Advanced Laparoscopic Cancer Surgeon
Hubli–Dharwad
📱 Phone: 9130056215